
Hello! My name is Gabriella Furfari. I’m a Physician Assistant at Trillium Creek Dermatology.
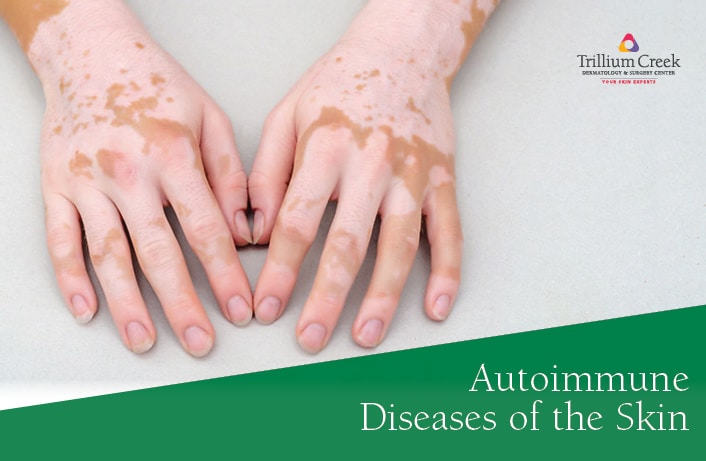
Autoimmune diseases occur when our own immune cells in our body attack our healthy cells. When our normal immune cells fail to differentiate between their own cells and begin attacking healthy cells, the skin, joints, and internal organs are affected. Many people may not even know they have an autoimmune skin disease and may not seek treatment. Some common autoimmune diseases that affect the skin include conditions such as psoriasis, vitiligo, lupus, hidradenitis suppurativa, bullous pemphigoid, and many others. The cause of why certain people acquire autoimmune diseases of the skin is not entirely understood, but there are several triggers that may predispose an individual. These include bacterial infections, drugs, allergens, and genetic factors. Signs and symptoms of autoimmune skin diseases include skin rashes, blisters, itchy lesions, hives, scaly patches, fatigue, or joint pain. A skin biopsy is usually indicated for a definitive diagnosis; however, many autoimmune diseases can be diagnosed on a clinical basis.
If you have been diagnosed with an autoimmune skin disease, you may need specific systemic therapeutics in order to manage your condition. These therapies target specific immunologic pathways by quieting an overactive immune system that lead to symptoms of your autoimmune disease. This can be life changing for some individuals who are unable to perform normal activities of daily living due to limitations from their autoimmune disease. It is important to know that most systemic therapies that we use in dermatology are generally considered safe in healthy individuals.
In addition to therapeutic agents, there are many lifestyle changes you can make to manage your autoimmune disease and prevent flares. According to researchers, quitting smoking, limiting alcohol use, reducing stress, and following a healthy diet can all help reduce symptoms of psoriasis and other autoimmune diseases. Researchers have also found that weight loss can even reduce your need for systemic therapy and reduce flares associated with autoimmune diseases such as psoriasis and hidradenitis suppurativa. Not only do all of these lifestyle changes help with your autoimmune disease, but they also help prevent comorbidities such as cardiovascular disease, high blood pressure, high cholesterol, depression, and obesity that may be associated.
Here at Trillium Creek Dermatology, our skin experts are fully knowledgeable in autoimmune skin diseases and we offer the best and latest treatment modalities available for our patients. Don’t let your autoimmune skin disease affect your quality of life. Make an appointment today with one of our dermatology providers.
To schedule an appointment, call us at 330.725.0569. We have five convenient locations in Brunswick, Medina, Strongsville, Wadsworth, and Wooster, OH.


