When your body’s natural defense system attacks healthy cells in your body, you are suffering from an autoimmune disorder. There are several common autoimmune diseases that affect the skin. These include vitiligo, scleroderma, lupus, psoriasis and vasculitis.
The exact reasons why our immune system becomes confused and starts to attack our own healthy cells is not entirely understood, but there appear to be genetic links where susceptibility and common symptoms to autoimmune disorders runs in families. It is also believed that exposure to certain bacteria, viruses, allergens and toxins can trigger the autoimmune condition. Diet and stress have also been implicated.
Our skin experts at Trillium Creek Dermatology carry out full assessments of skin conditions and provide a variety of treatments to manage the skin and minimize the visible effects and damage due to autoimmune disorders.
Autoimmune Disorders List
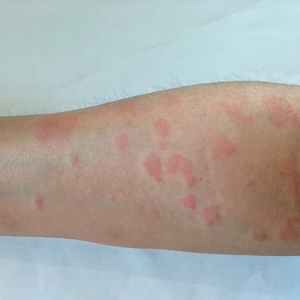
Lupus
Primarily affecting women of child-bearing age, lupus is a serious autoimmune disease. It is estimated that 1.5 million people in the US suffer from lupus. When the disease is most active it can affect the whole body, including the skin, joints, kidneys, heart, lungs, blood vessels and brain.
Learn More
Scleroderma
Thick areas of skin with a smooth shiny appearance are a defining feature of scleroderma. This is a group of connective tissue disorders that cause a thickening and hardening of the skin (a process known as fibrosis). Blood vessels can also become damaged and the body is unable to repair them. Scleroderma usually starts with a few dry patches of skin on the hands or face that then become thicker and harder. These patches then spread to other areas of the skin.
Learn More
Vasculitis
As the name suggests, vasculitis is a serious condition involving inflammation of the blood vessels when the body’s immune system attacks them. Inflammation can be short-term (acute) or long-term (chronic), and in severe cases blood flow can be restricted to such an extent that organ and tissue damage occurs.
Learn More
Vitiligo
Vitiligo is a pigmentation disorder in which your skin loses melanin, causing white patches to appear that slowly enlarge over time. These symptoms affect men and women alike, and causes may be attributed to emotional stress, illness or skin trauma such as sunburn. Vitiligo can appear from birth but half of all vitiligo cases develop in children and young adults between the ages of 10 and 30 years.
Learn More

